The current edition of the journal Experimental Dermatology is featuring many articles on the functions of subcutaneous (beneath the skin) adipose cells (fat cells). These cells are involved in numerous functions. The articles suggest that the negative health effects of unnecessary loss of body fat – on the part of some women influenced by skinny high-fashion models – are greater than what most would assume.
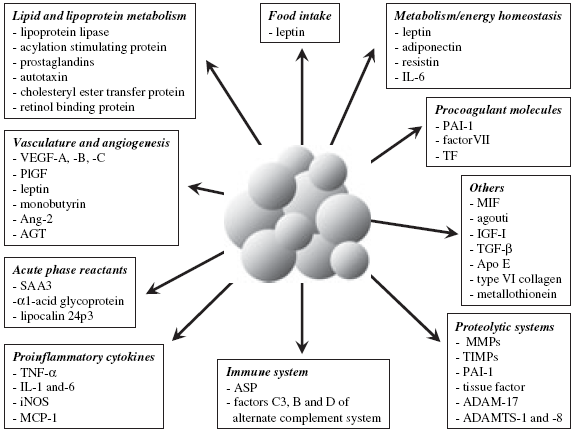
The following figure sums up the major body functions influenced by fat cell-derived factors, making it clear that both too little and too much subcutaneous fat is going to be bad for health.
Legend: "Overview of the major functions modulated by adipocyte-derived factors. ADAM, a disintegrin and metalloprotease; ADAMTS, a disintegrin and metalloproteinase with thrombospondin motifs; AGT, angiotensinogen; Ang-2, angiopoietin-2; Apo E, apolipoprotein E; ASP, acylation stimulating protein; IGF-I, insulin-like growth factor-I; IL, interleukin; iNOS, inducible nitric oxide synthase; MCP-1, monocyte chemotractant protein-1; MIF, macrophage migration inhibitory factor; MMP, matrix metalloprotease; PAI-1, plasminogen activator inhibitor-1; PlGF, placenta growth factor; SAA3, serum amyloid A3; TF, tissue factor; TGF-b, transforming growth factor-b; TIMP, tissue inhibitor of MMP; TNF-a, tumor necrosis factor-a; VEGF, vascular endothelial growth factor."
Some of the commentary talks about the historical/cultural change involving the “ideal female silhouette,” but the authors’ views are naïve. The authors use the examples of the morbidly obese Venus of Willendorf, Aphrodite Callipygos, Peter Paul Rubens’ obese women and Kate Moss. Venus of Willendorf from Paleolithic Europe cannot be assumed to represent a figure held in the “highest esteem”; the figurine is probably a fertility symbol. Most female figurines from Neolithic Europe are not overweight/obese. Aphrodite Callipygos simply represents a well-developed feminine backside in a woman within the medically normal weight range. Peter Paul Rubens’ paintings of obese women notwithstanding, there was stigma against obesity in medieval Europe. And, the typical skinniness of high-fashion models is not held as an ideal by most people in Western societies; this ideal is primarily held by some girls/women who are misled by the high status of high-fashion models and gay fashion designers who believe that the typical [non-overweight] physique of 13-year-old boys is hot. Historical changes in the representation of the female form need to be addressed in some detail, but this is not the entry to do it.
The prelude is reproduced below, and the others are available as a pdf file.
What are subcutaneous adipocytes really good for…?
Ralf Paus, J. Klein, P. A. Permana, M. Owecki, G. N. Chaldakov, M. Böhm, G. Hausman, C. M. Lapière, P. Atanassova, J. Sowiński, M. Fasshauer, D. B. Hausman, E. Maquoi, A. B. Tonchev, V. N. Peneva, K. P. Vlachanov, M. Fiore, L. Aloe, A. Slominski, C. L. Reardon, T. J. Ryan, C. M. Pond, Terence J. Ryan.
Experimental Dermatology 16 (1), 45–47 (2007).
doi:10.1111/j.1600-0625.2006.00519_1.x
Abstract: Our acute awareness of the cosmetic, psychosocial and sexual importance of subcutaneous adipose tissue contrasts dramatically with how poorly we have understood the biology of this massive, enigmatic, often ignored and much-abused skin compartment. Therefore, it is timely to recall the exciting, steadily growing, yet underappreciated body of evidence that subcutaneous adipocytes are so much more than just 'fat guys', hanging around passively to conspire, at most, against your desperate attempts to maintain ideal weight. Although the subcutis, quantitatively, tends to represent the dominant architectural component of human skin, conventional wisdom confines its biological key functions to those of energy storage, physical buffer, thermoregulation and thermoinsulation. However, already the distribution of human superficial adipose tissue, by itself, questions how justified the popular belief is that 'skin fat' (which actually may be more diverse than often assumed) serves primarily thermoinsulatory purposes. And although the metabolic complications of obesity are well appreciated, our understanding of how exactly subcutaneous adipocytes contribute to extracutaneous disease – and even influence important immune and brain functions! – is far from complete. The increasing insights recently won into subcutaneous adipose tissue as a cytokine depot that regulates innate immunity and cell growth exemplarily serve to illustrate the vast open research expanses that remain to be fully explored in the subcutis. The following public debate carries you from the evolutionary origins and the key functional purposes of adipose tissue, via adipose-derived stem cells and adipokines straight to the neuroendocrine, immunomodulatory and central nervous effects of signals that originate in the subcutis – perhaps, the most underestimated tissue of the human body. The editors are confident that, at the end, you shall agree: No basic scientist and no doctor with a serious interest in skin, and hardly anyone else in the life sciences, can afford to ignore the subcutaneous adipocyte – beyond its ample impact on beauty, benessence and body mass.
Prelude 1
Adipose tissue has been neglected and misunderstood, at least in man (for it has long been known to be an energy resource for rats). What would women's journals write about if they had not heard of 'cellulite'? Even though they have got it wrong, 'Cellulite' is an 'invented disease' that only reflects a weak and aging dermis which allows fat to protrude and make the surface lumpy bumpy.
The long known functions of fat are listed in Table 1, and their relevance to the skin is reviewed elsewhere (1). More recently known are endocrine and cytokine production and the role of adipose tissue as a resource for stem cells.
Table 1. Functions of adipose tissue. |
| Emergy provision |
| Thermoregulation |
| Insulation |
| Body contour |
| Endocrine |
| Cytokine and growth factor generation |
| Stem cells |
| Fatty acids for cell membranes and other specific functions of host and infective organisms |
But none of that explains the presence of all that fat, e.g. in the omentum or around lymph glands in the groin. Neither does it explain why antiviral therapy in HIV/AIDS causes havoc with body shape, with some sites atrophying and others showing disfiguring hypertrophy. Why is bone marrow replaced by fat cells as it ages, or why do lipomata arise sometimes from haematomata? Why do 100 000 000 persons accumulate fat in their lymphoedematous limbs (2)?
The questions continue: Why is so much tropical disease affecting the skin, focused on fat (3)? How come that the causative organism of leprosy lost most of that part of its genome that deals with lipid-metabolizing lipases and favours a dendritic cell that hugs the fatty myelin of nerves (4)? Why does the causative organism of the Buruli ulcer localize in adipose tissue (5)?
I have raised a question about the fat cells that are localized around adnexa and could favour bacteria inoculated by biting insects (3). Is the answer that stored in fat are a range of fatty acids any one of which is specifically and essentially required by at least one tropical organism? One no longer hypothetical example is the trypanosome of Chagas' disease which finds its specific fatty acid needs in the heart (6). I have asked whether the filaria of lymphatic filariasis choose the collecting lymphatics of the groin to grow microfilaria (is it because only there are the essential fatty acids they need, which are continually produced to feed the specific needs of inguinal lymphoid tissue?) (3).
It is Caroline Pond and her colleagues who have raised some of the most controversial issues in the adipose tissue fraternity (7–9). They say that dendritic cells and much of our immune system require very specific fatty acids and must induce a supply in their immediate neighbourhood. They do this by having control of the generation of fat and determining its fatty acid content and type.
Certain diseases are examples of an associated excessive induction of too great an amount of adipose tissue. They include exophthalmus, and Crohn's disease (10), the latter a clear example of lymphoid tissue associated with excess fat cells.
All of this exciting controversy is made more convincing by the realization that our ancestors made better use of fat to feed an immunosurveillance system (11). The earthworm's skin fights off earthen threats by using its skin and, thus, can do without a lymphatic system with lymph nodes to help recognize what is foreign and undesirable. Even earlier unicellular organisms evolved the cell membrane composed of cholesterol and phospholipids to incorporate proteins, fats and carbohydrate swinging between the cytosol and the external environment to help identify its needs and dislikes - a capacity that contemporary human biology has preserved in its own basic cellular structure and behaviour.
Now we have an epidemic of obesity that some believe is an inflammatory state and witness an era of detection and understanding of ancient cytokines. Apparently, it is tumor necrosis factor-α that helps to understand cachexia and weight loss in HIV/AIDS(12,13).
It is the contemporary generation of knowledge of genetics, growth factors and cytokines that almost daily turns our attention to the shamefully neglected role of stored fat.
Why should an inactivating mutation of VEGFR-3, which was first studied because it is linked to lymphatic function, produce obesity in a mouse (14)? Why should Prox1, a key transcription factor in lymphatic development, do the same (15)?
Energy production by lipase breakdown of fat storage is a 'common strategy' in a world of 'infrequent nutrient supply' (16). Dermatologists should ask why mutations in the catabolism of neutral lipid by lipases cause one genetic variant of ichthyosis (17). Unravelling this exposes complex interactions: for example, such interactions may also explain the acanthosis nigricans of some insulin-resistant conditions or the bizarre acanthosis of elephantiasis, which may perhaps have to do more with membrane remodelling rather than with energy production, and may be subject to the influence of catecholamines on adenyl cyclase and protein kinase A and cyclic AMP.
The epidermis needs fat (18) and dermatologists have long ignored that local availability of fat determines fast keratinization and several skin functions depend on it (1). Hence, specialised adnexa, the hair follicle, whisker and antler when attached to the sub-cutaneous tissue grow keratin, and its bloodsupply, under the influence of sex hormones, at a great rate.
Adipose cells are a gross example of lipid droplets, and their containment is everything but simple (17). There are several genes whose sole function is to regulate the surface proteins (appropriately named perilipins) on such droplets, which determine how droplet content is made available for metabolism.
I have long held that dermatologists give little credit and prefer not to own adipose tissue, just as when I began my career they foolishly ignored blood vessels and later the lymphatics. The skin is peculiar in that, in health, it is mostly living without consuming oxygen. The epidermis is almost anaerobic. When it is in repair mode, however, switched on e.g. by transepidermal water loss and almost any injury, it becomes a factory for inflammatory mediators recruiting oxygen-demanding cells such as the neutrophil and oxygen-consuming activities such as mitosis and migration. It has to ensure adequate blood supply for repair and even makes a new organ known as granulation tissue. It does this while creating an improved lymphatic drainage system linked to macrophages and lymphoid cells with an immunosurveillance role. This process involving VEGF and hypoxia-inducing regulation of adipogenesis (19) results eventually in granulation tissue being turned into adipose tissue. It is surely possible that the demands of repair exceed supply in many forms of hyperkeratosis and parakeratosis. Likewise, chronic hypoxic injury inducing fatty acid release deserves investigation.
One other neglected theme is skin temperature – which is habitually low and similar to the metabolism of hibernation. Here, too, fat metabolism has much to tell us. The tropical diseases mentioned above, leprosy, Buruli ulcers, lymphatic filariasis or 'organs' such as granulation tissue would be best understood if all studies of the skin adopted temperatures that were lower than the core temperature of 37°C.
Now that dermatologists have become cosmetologists sucking out adipose tissue and placing it elsewhere with crude technology, enhancing the least of the fat cell functions to support body contour, they never think deeply about the cells on which they are practising genocide. Let me conclude this overture to a fascinating controversy in experimental dermatology, therefore, by reminding us that these abused cells have the potential to create an entire human being and that more careful dissection of their metabolism may help us to explain a majority of skin diseases.
References
- Ryan T J, Curri S. The Cutaneous Adipose Tissue. In: Dermatology Clinics. Philadelphia, PA: J B Lippincott, 1989: 7: 1–163.
- Ryan TJ. Lymphatics and adipose tissue. In: Ryan T J, Mortimer P S, eds. The Cutaneous Lymphatic System. Clin Dermatol 1995: 13: 493–498.
- Ryan T J. Lymphology 2006: 39: 49–52.
- Gordon S V et al. Trans R Soc Trop Med Hyg 2002: 96: 1–6.
- Wansbrough-Jones M, Phillips R. Br Med J 2005: 350: 1402–1403.
- Coombs T P et al. J Biol Chem 2005: 280: 24085–24094.
- Mattacks CA et al. Lymphat Res Biol 2004: 2: 107–129.
- Mattacks C A et al. Adipocytes 2005: 1: 43–56.
- Pond C. Prostaglandins Leukot Essent Fatty Acids 2005: 73: 17–30.
- Westcott E et al. Inflamm Bowel Dis 2005: 11: 820–827.
- Caspar-Bauguil S et al. FEBS Lett 2005: 579: 3487–3492.
- Grunfeld C, Feingold K. New Engl J Med 1992: 327: 329–337.
- Price S R M et al. Biochem Biophys Acta 1986: 889: 374–381.
- Karkkainen M J et al. Proc Natl Acad Sci U S A 2001: 98: 12677–12682.
- Harvey N L et al. Nat Genet 2005: 37: 1072–1081.
- Lass A et al. Cell Metab 2006: 3: 309–319.
- Haemmerle G et al. Science 2006: 312: 734–737.
- Rawlings A V, Matts P J. J Invest Dermatol 2005: 124: 1099–1110.
- Yun Z et al. Dev Cell 2002: 2: 331–341.
Comments
Subcutaneous fat is an organ, not a demon to be exorcised Hollywood-style (unlike visceral fat, which actively functions in a destructive manner, which should be exorcised with exercise).
I skimmed the science bits, so if this aspect of health was included, sorry--I may have missed it: subcutaneous fat produces estrogen in both men and women. Females are at higher risk for osteoporosis, however, so the suppression of normal-range hormone levels by being underweight for extended periods increases the risk of this degenerative disease manifold. The probability that women are prone to excessive weight consciousness during their most important years for increasing bone density means that this androgynous-model-idealization won't be merely a harmless phase for those women who manage to grow out of it.
Hi, this is interesting but! I'd be interested to see a piece on why a lot of straight men DO like very very thin and waif-like girls. I have several male friends (who are almost all white) that only exclusively date skinny girls. Just based on the anecdotal evidence these guys are usually pretty feminine and skinny themselves.
This is so stupid give some straight forward answers
ACUSE ME THIS IS THE CORRECT Answers for anything u would of asked that is related to this
It is common knowledge the excessive adipose tissue may bring health issues. Best thing to do is to stay in shape and allow no excesses. I have met people that display different reactions under stress and pressure. Some of them eat in average quantities and, unexpectedly, keep losing weight. These are serious signs to be taken into account and maybe ask for some medical advice concerning an eating disorder treatment. There`s no hopeless situation, things will get back to normal in no time.
This article sucks it is way to long but the information in a shorter form. Who wants to sit and read very long papragarphs that are so long they dont make sense!!!!!!